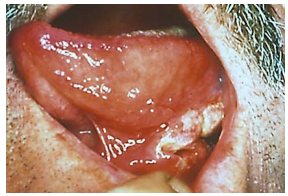
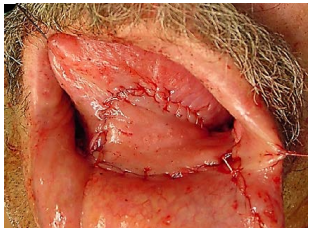
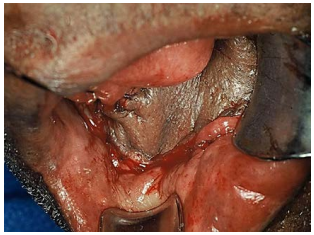
Cancers of the floor of the mouth (FOM) are generally treated with primary surgical resection (Figures 1 & 2). Adjuvant irradiation is indicated for advanced tumours, tumours with perineural invasion (PNI) or uncertain/close margins.

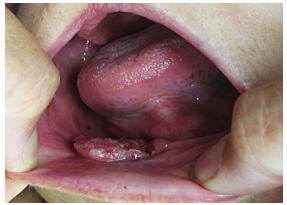
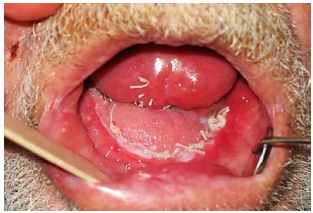
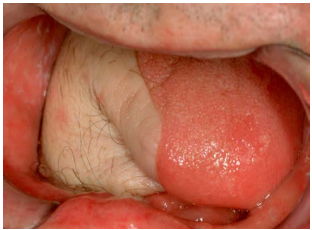
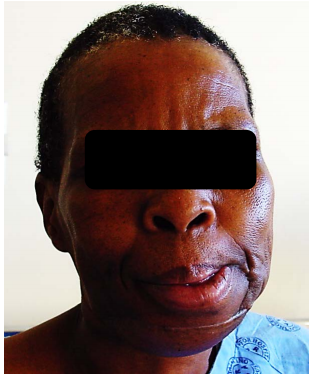
Resection of cancers of the FOM without taking cognisance of oral function may severely cripple the patient in terms of speech, mastication, oral transport and swallowing. Resecting the anterior arch of the mandible beyond the midline without reconstructing the bone with loss of the anterior attachments of the suprahyoid muscles (digastric, geniohyoid, mylohyoid, genioglossus) leads to an Andy Gump deformity with loss of oral competence, drooling, and a very poor cosmetic outcome (Figure 3).

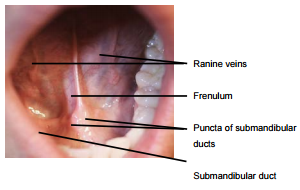
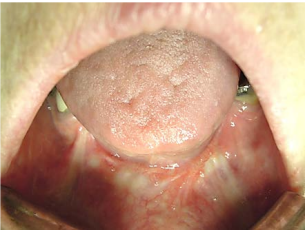
The FOM is a horseshoe-shaped area that is confined peripherally by the inner aspect (lingual surface) of the mandible. It extends posteriorly to where the anterior tonsillar pillar meets the tonsillolingual sulcus, and merges medially with under-surface of the oral tongue. It has a covering of delicate oral mucosa through which the thin walled sublingual/ranine veins are visible. The frenulum is a mucosal fold that extends along the midline between the openings of the submandibular ducts (Figure 4).
The mylohoid muscle forms the diaphragm of the mouth and separates the FOM from the submental and submandibular triangles of the neck (Figures 5, 6, 7).
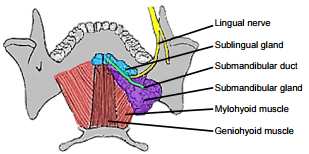
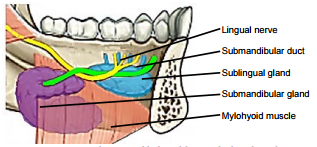
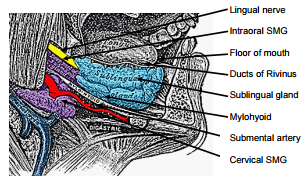
The following structures are located between the mucosa and the mylohyoid muscle: paired geniohyoid muscles in the midline (Figure 5); sublingual salivary glands (Figures 5, 6, 7), submandibular ducts (Figures 5, 6), oral component of submandibular salivary glands (Figures 5, 6, 7), genioglossus muscle (Figure 8), and the lingual (Figures 5, 6, 7) and hypoglossal nerves (Figure 8).
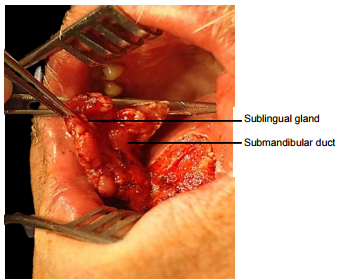
The paired sublingual salivary glands are located beneath the mucosa of the anterior floor of mouth, anterior to the submandibular ducts and above the mylohyoid and geniohyoid muscles (Figures 5, 6, 7). The glands drain via 8-20 excretory ducts of Rivinus into the submandibular duct and also directly into the mouth on an elevated crest of mucous membrane called the plica fimbriata which is formed by the gland and is located to either side of the frenulum of the tongue (Figures 6, 7).
The submandibular duct is located immediately deep to the mucosa of the anterior and lateral FOM, and opens into the oral cavity to either side of the frenulum (Figures 4, 5, 6).
The lingual nerve provides sensation to the floor of the mouth. It crosses deep to the submandibular duct in the lateral floor of mouth (Figures 5, 6, 7). In the anterior FOM it is located posterior to the duct (Figure 5).
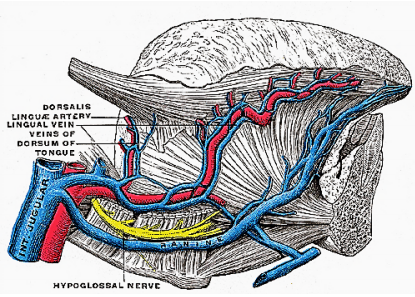
Ranine veins are visible on the ventral surface of the tongue, and accompany the hypoglossal nerve (Figures 4, 8).
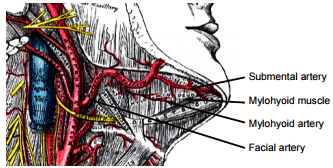
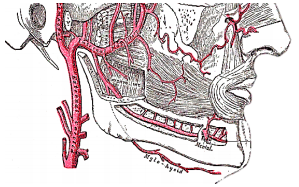
Arterial supply to the tongue and FOM is derived from the lingual artery and its branches (ranine artery, dorsalis linguae, and sublingual arteries) (Figures 8, 9); and the mylohyoid and submental branches of the facial artery.
The lingual artery arises from the external carotid artery between the superior thyroid and facial arteries and courses obliquely forwards and medial to the greater cornu of the hyoid (Figures 8, 9).
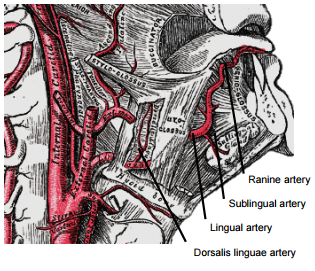
It then loops downward and anteriorly and crosses medial to XIIn and the stylohyoid muscle. It then courses directly anteriorly below hyoglossus and finally ascends as the ranine artery (profunda linguae) submucosally on the undersurface of the tongue as far as its tip; it lies to either side of the genioglossus, and is accompanied by the lingual nerve. Two or three small dorsales linguæ arteries arise beneath the hyoglossus and ascend to the posterior part of the dorsum of the tongue and also supply the mucous membrane of the posterior FOM, and oropharynx. The sublingual artery arises from the lingual artery at the anterior edge of the hyoglossus and runs forward between the genioglossus and mylohyoid and supplies the sublingual salivary gland and mucous membrane of the FOM and gingiva (Figures 8, 9). A branch of the sublingual artery pierces the mylohyoid muscle and anastomoses with the submental branch of the facial artery.
The submental branch of the facial artery courses along the inferior, inner margin of the mandible (Figures 10). The mylohyoid artery and vein are encountered when the surgeon elevates the submandibular gland from the lateral surface of the mylohyoid (Figures 10 & 11). It branches from the inferior alveolar artery just before it enters the mandibular foramen, crosses the mylohyoid, and disappears anteriorly behind the digastric. It has connections with the submental artery, and via a defect in the mylohyoid with the sublingual artery in the floor of the mouth.
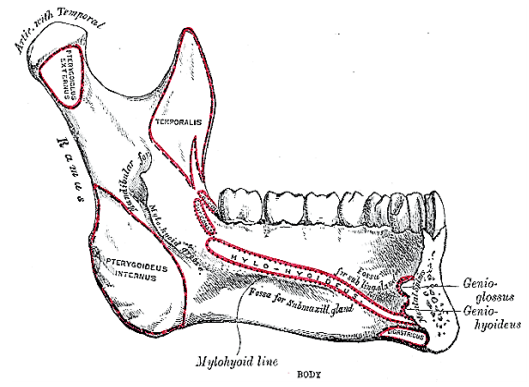
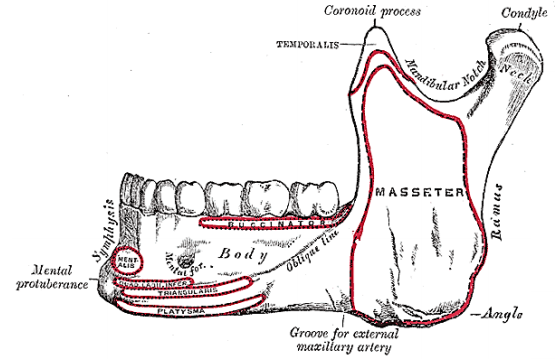
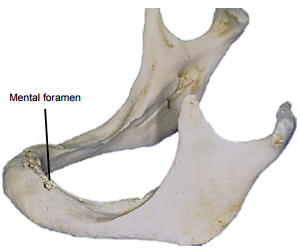
The mandible forms the peripheral border of the FOM, and may be involved by FOM tumours or may have to be divided (mandibulotomy) or resected (alveolectomy / marginal mandibulectomy / segmental mandibulectomy / hemimandibulectomy). Important surgical features are the position of the mental foramina through which the mental nerves exit to innervate the lower lip, the mylohyoid line to which the mylohyoid muscle attaches, and when planning a marginal mandibulectomy, the height of the body of the mandible and the depth of the dental roots (Figures 12a, b).
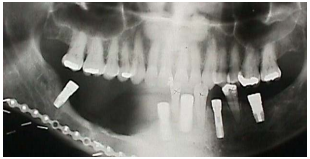
The mental foramen and inferior alveolar nerve may be very close to the superior surface of a resorbed mandible such as is seen in older, edentulous patients (Figure 13). A marginal mandibulectomy may also not be possible in such a resorbed mandible due to the lack of residual bone.
Surgical Objectives
The author advocates elective neck dissection (END) levels I-IV for squamous cell carcinomas that are >4mm thick and/ or >T2 stage. A useful rule of thumb is that a palpable tumour is likely to have a tumour thickness that warrants END. Tumours of the anterior FOM that approach the midline require bilateral END.
The remainder of this chapter will focus on the surgical treatment of the primary tumour.
Preoperative evaluation
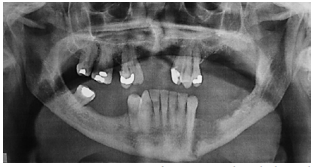
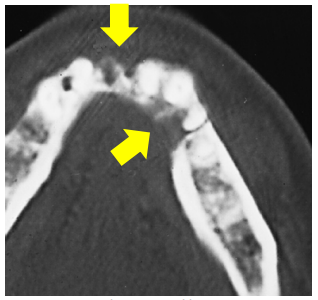
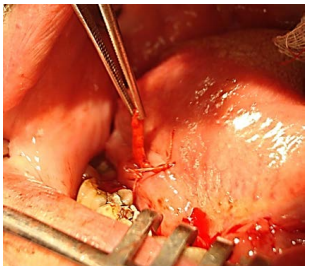
Nasal intubation is followed by tracheostomy. Perioperative antibiotics are administered.
Transoral: Smaller tumours (T1-T2) are usually easily excised though the open mouth in an edentulous patient. The mouth is kept widely open either with a dental bite bock (Figure 17) or with a self-retaining retractor taking care to protect the teeth (Figure 18)
However, resecting an anterior FOM tumour may be quite challenging in a patient with a full set of lower teeth as the teeth may obstruct access to the anterior FOM. In such cases lower teeth may need to be extracted and a marginal mandibulectomy (Figure 19) or a mandibulotomy may be required for access.
When a FOM tumour abuts the anterior mandible then doing a marginal mandibulectomy in continuity with the tumour resection greatly facilitates resection by freeing up the tumour.
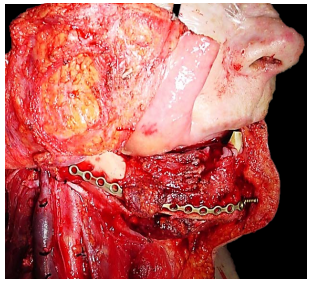
Midline lip-split: The lip is split in the midline after scoring/marking the vermillion border so as to ensure an accurate repair. The soft tissues are stripped off the front of the mandible (Figure 20).
Visor flap: This is achieved by cutting along the gingivolabial and gingivobuccal sulci about 1cm from the bone so as to permit placement of sutures when closing the wound, and then stripping the soft tissues from the outer aspect of the mandible. Take care not to transect the mental nerves if they can be saved. The skin flap is then retracted superiorly to expose the mandible (Figure 21).
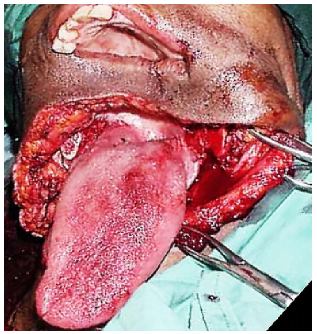
Pull-through: This may be employed when the tumour stops some distance from the inner aspect of the mandible. Following bilateral neck dissections of Levels 1a and 1b, the mandibular attachments of the anterior bellies of digastric, mylohyoid, geniohyoids and genioglossus are divided with electrocautery working from inferiorly (Figure 12a). The mucosa of the anterior FOM is then divided 1cm from the inner aspect of the mandible (so as to facilitate later repair). This permits the surgeon to deliver the anterior FOM and anterior tongue into the neck and then to proceed with the resection.
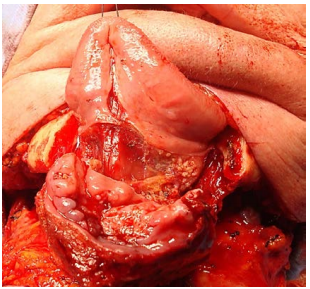
First complete Levels 1a and b of the neck dissection(s) before proceeding to the resection. This permits the surgeon to cut through the muscles in the FOM and tongue knowing the location of the XIIn, lingual nerve and lingual artery.
Mandibulectomy: If a marginal or segmental mandibulectomy is planned then it should be done before resecting the FOM tumour as it improves surgical exposure (Figure 21). If a segmental mandibulectomy is to be done, then preplate the mandible with a reconstruction plate so as to ensure alignment of the teeth and a good bony contour (Figure 20). Marginal mandibulectomy is done with small sharp osteotomes so as to avoid inadvertent fracture of the mandible, or with a powered oscillating or reciprocating saw. With marginal mandibulectomy the cut is made obliquely so as to preserve the height of the outer cortex for mandibular strength, but to remove the inner cortex that abuts the tumour. With segmental mandibulectomy the bone is cut at least 2cm from visible tumour (Figure 21).
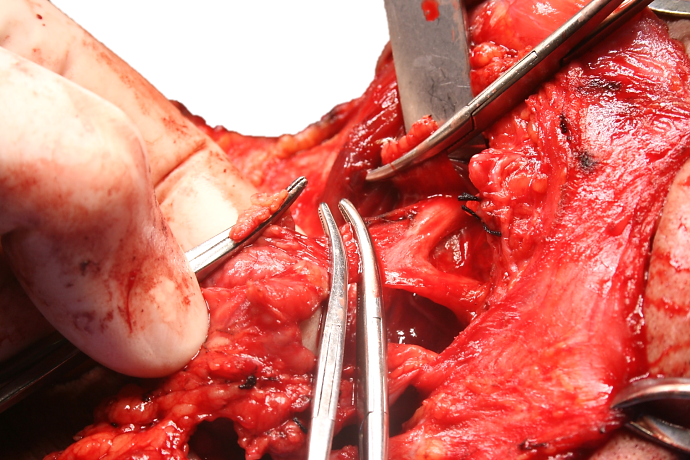
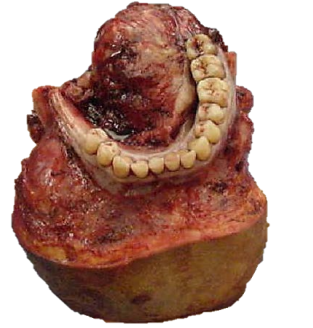
Tumour: Once the mandibulectomy has been completed, keep the bone attached to the tumour specimen and divide the gingival mucosa on the inside of bone cuts; this will release the tumour from bone and facilitate delivery of the tumour into the surgical field. Identify and preserve the submandibular duct(s), and the lingual and hypoglossal nerve(s) if possible. The sublingual gland may be encountered in anterior FOM cancer resections (Figure 18).
Use diathermy to resect the tumour with at least 1cm margins. Cauterise the ranine vessels during the resection. Larger branches of the lingual artery are ligated as they are encountered. Obtain frozen section confirmation of clear tumour margins if available.
Following resection the surgeon carefully assesses the defect to determine how best to restore form and function i.e. mandibular integrity and contour, and oral competence, mastication, oral transport, swallowing and speech.
No repair: Small and/or superficial resections above the mylohyoid that do not communicate with the neck dissection may be left open to heal like a tonsillectomy wound. Resist the temptation to suture such defects as it may alter the shape of the tongue or fix the tongue to the anterior FOM.
Primary closure: Avoid tethering or distorting the tongue. Note the comment about marginal mandibulectomy above (Figure 19).
Split skin graft: This may be used to cover a defect that could otherwise be left open but for concern about a through-and-through communication to the neck, or over a marginal mandibulectomy defect (Figure 22). The skin is sutured to the margins of the defect with absorbable sutures, the ends of which are left a few centimetres long. A bolster of antiseptic-impregnated gauze is placed over the skin graft and tied down with the long sutures. The bolster is removed after about 5 days.
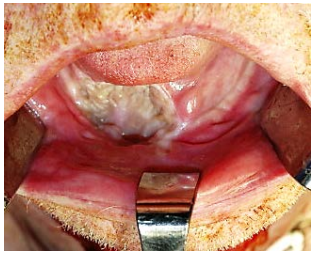
Buccinator myomucosal flap: (Figures 23a,b,c) This is an excellent flap for both anterior and lateral FOM defects as it has the same physical qualities as tissues of the FOM. The pedicle however has to cross the mandible and is therefore best suited for edentulous patients, patients with missing teeth, or who have undergone marginal mandibulectomy. (See chapter: Buccinator myomucosal flap)
Nasolabial flap: The nasolabial flap can be used both for lateral and anterior FOM defects (Figures 24, 25) (See chapter: Nasolabial flap for oral cavity reconstruction)
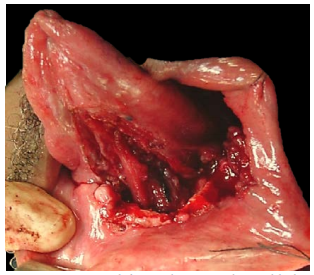
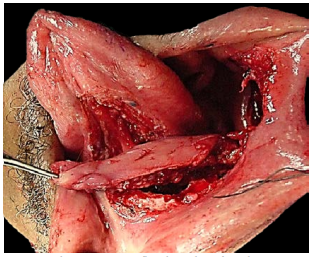
Pectoralis major flap: This flap is only used if other flaps listed are not available. (See chapter: Pectoralis major flap)
Radial free forearm flap: This is a popular choice for FOM repair as the flap is thin and pliable. An osseocutaneous flap can be used as an onlay graft with marginal mandibulectomy defects (Figure 26a, b) (See chapter: Radial free forearm flap)
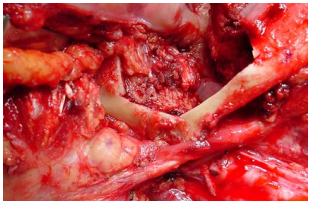
Anterolateral free thigh flap: (Figure 27) Muscle harvested with the flap can be tailored according to the volume of the defect to be filled. However it is less pliable than the radial free forearm flap and is only suitable for oral reconstruction in patients with thin thighs.
Free fibula flap: This is the workhorse of mandible reconstruction following segmental mandibulectomy (Figures 28 a-c). but can also be used as an onlay flap. It is also suitable for dental implants (Figures 29a, b). (See chapter: Free fibula flap)
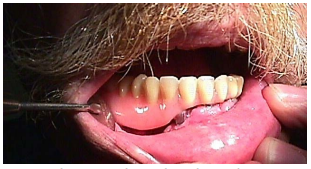
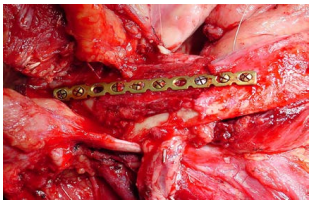
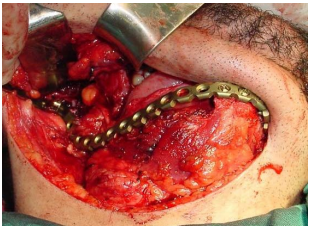
Titanium reconstruction plate: Although it can be used to replace mandible, it is prone to extrusion both to the inside of the mouth and through skin (Figure 30).
Resecting tumours of the FOM is challenging particularly in terms of optimising oral function. The surgical team has to master a wide array of reconstructive techniques so as to secure the best functional and cosmetic outcomes.
Johan Fagan MBChB, FCORL, MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town
South Africa
johannes.fagan@uct.ac.za