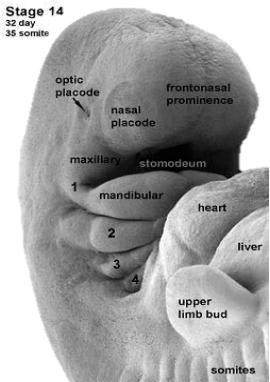
Failure of a branchial cleft to involute may manifest as an epithelial-lined cyst, sinus or fistula. Sinuses open either onto the skin, or into the oro- or hypopharynx.
Branchial anomalies may be diagnosed at any age but present most commonly in infancy and childhood as a cutaneous sinus, a cyst or an abscess. The differential diagnosis of a cystic lateral neck mass includes thymic, parathyroid and thyroid cysts, cystic metastases (papillary thyroid carcinoma, oropharyngeal squamous cell carcinoma, skin cancer), tuberculous cold abscess, lymphatic malformation, plunging ranula, and laryngocoele. The existence of branchiogenic carcinoma is controversial. Cystic metastases to cervical lymph nodes originating from oropharyngeal squamous cell carcinoma occur far more commonly and should be suspected particularly in adult patients presenting with cystic masses in Levels 2 or 3 of the neck.
Surgical excision is the standard of care. An understanding of the embryology of the branchial apparatus is required to diagnose and operate on such patients.
Embryology
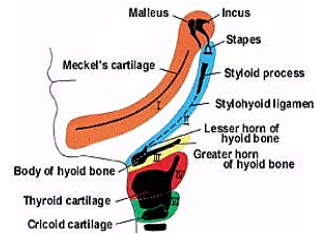
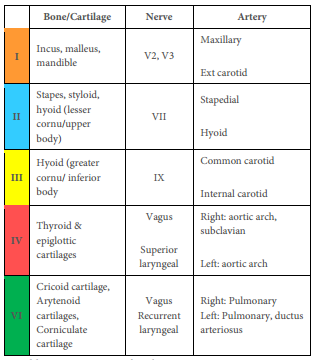
The branchial apparatus develops during the 2nd - 6th weeks of life. At this stage the neck of the foetus is shaped like a hollow tube with circumferential ridges called branchial arches which are separated internally by branchial pouches and externally by clefts (Figure 1). It is lined by ectoderm externally and endoderm internally; mesoderm and neural crest cells migrate into the branchial arches to evolve into musculoskeletal, vascular and cranial nerves that serve the structures of that arch (Figure 2). The endoderm that lines the branchial pouches evolves into the middle ear, tonsil, thymus and parathyroid (Figures 3, 4). The 1st branchial cleft evolves into the external auditory meatus (Figure 3).

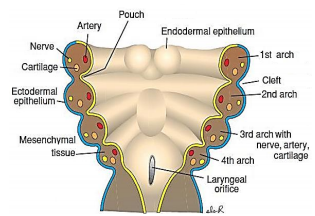
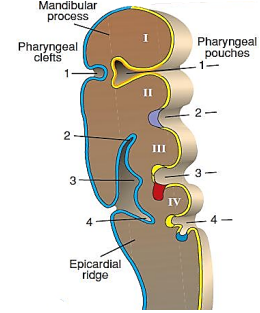
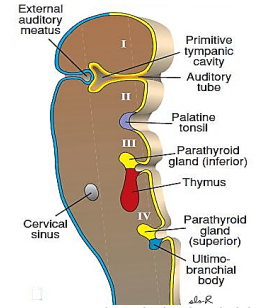
The 2nd - 4th clefts form a common cavity called the Sinus of His with a single external opening (Figure 3). The 2nd arch subsequently grows inferiorly and covers the Sinus of His to give rise to a single branchial cleft cyst called the cervical sinus which subsequently involutes (Figure 4). Should a branchial cleft or the Sinus of His persist, it results in an epithelium-lined branchial cyst or sinus. Because clefts 2 - 4 embryologically have a common external opening, one cannot determine the cleft of origin by the position of the external sinus. A sinus may also result from spontaneous drainage of a cyst onto the skin or pharyngeal mucosa or following incision and drainage. A fistula results from a communication between a branchial cleft and pouch.
Branchial anomalies lie caudad to the embryologic derivatives of the associated arch and cephalad to the derivatives of next arch (Figures 4, 5, Table 1).
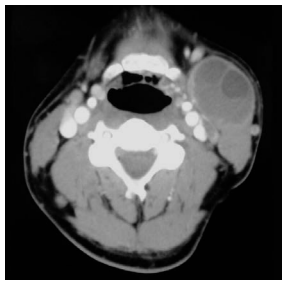
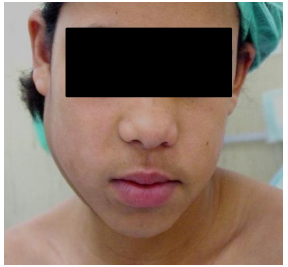
A cyst may present as an external swelling, or cause dysphagia or airway obstruction due to its mass effect, or become infected and present as an abscess (Figures 7, 8).
Cutaneous sinuses and fistulae present along the anterior border of the sternocleidomastoid muscle.
1st branchial cleft anomalies are uncommon and result from incomplete closure of the ventral part of the 1st branchial cleft. The 1st branchial cleft evolves into the external auditory canal; the pouch into the middle ear cavity, mastoid air cells and eustachian tube (Figures 4, 5); Work divided 1st branchial cleft anomalies into Types 1 & 2 (Laryngoscope 1972;82:1581-93).
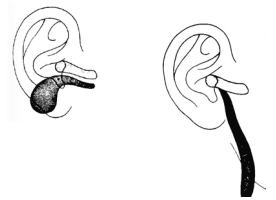
This is a duplication of the external auditory canal and is lined by squamous epithelium (Figure 9). It runs parallel to the ear canal and may have a fistula terminating in the postauricular or pretragal regions. It generally does not involve the VIIn. Treatment is by surgical excision of the cyst or fistula and of involved skin and cartilage of the external auditory canal.
This typically presents as a cyst / sinus / fistula, or combinations thereof. It is of both ectodermal and mesodermal origin and hence may contain skin, adnexia and cartilage. It extends between the angle of the mandible and the external auditory canal. The cyst or the external opening is typically located in the neck superior to the hyoid bone i.e. the next branchial arch (Figures 10, 11).
It crosses the angle of the mandible, courses through parotid and terminates near the bony-cartilaginous junction of the external auditory canal (Figures 9, 11-13).
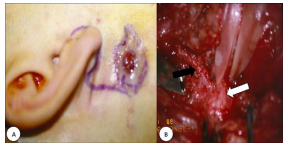
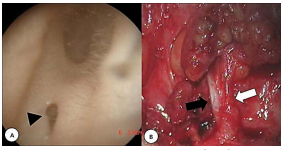
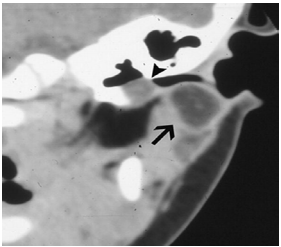
A surgeon should not embark on such surgery without being comfortable with operating on the VIIn, as the VIIn is associated with the 1st branchial arch, and is intimately associated with 1st branchial cleft anomalies; the tract may pass deep, lateral or between branches of the nerve, or a cyst may displace the nerve caudally.
Carefully examine the external ear canal with a diagnostic microscope for the presence of a sinus opening in the floor of the ear canal (Figure 12). Request CT +/ MRI to determine the anatomical relationships with the ear canal, parotid and VIIn; the position of the nerve can be estimated according to the position of the retromandibular vein relative to the anomaly.
Treatment is by surgical excision; this requires identification and preservation of the VIIn, partial parotidectomy, and excision of skin and cartilage of the external auditory canal around the tract:
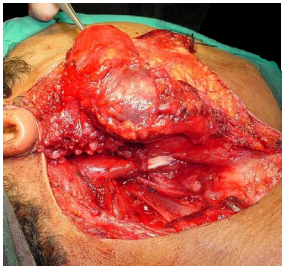
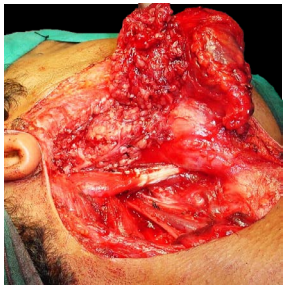
More than 90% of branchial anomalies arise from 2nd branchial clefts. The 2nd branchial arch contributes to the development of the hyoid; the cleft forms the Sinus of His jointly with clefts 3 and 4, and subsequently involutes; and the pouch becomes the palatine tonsil and supratonsillar fossa. Consequently 2nd arch anomalies communicate with the oropharynx via the supratonsillar fossa (Figures 15 - 17).
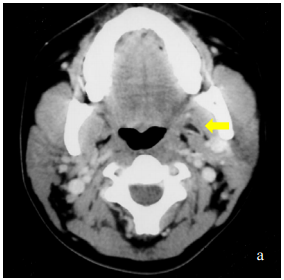
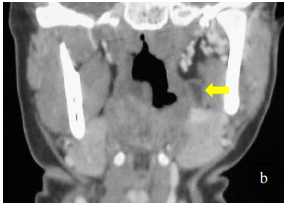
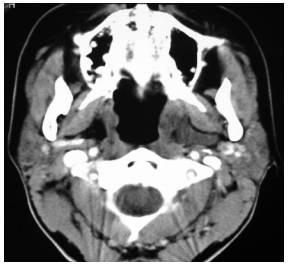
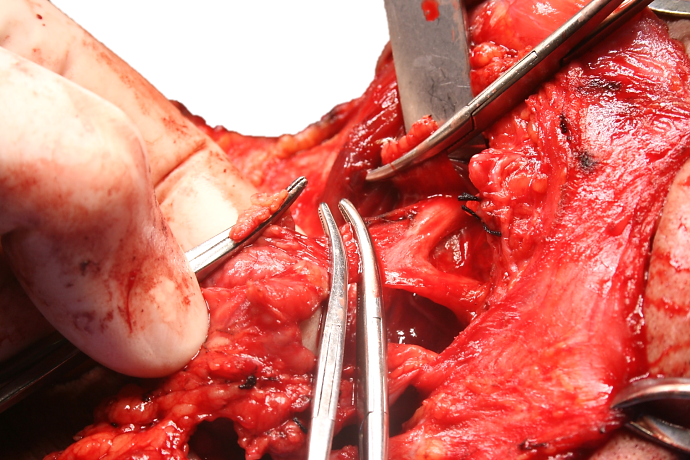
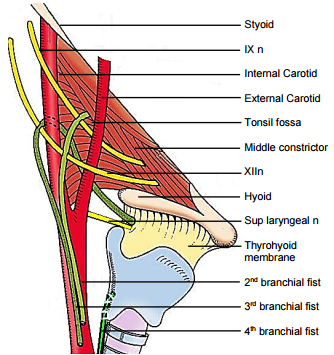
Like 3rd and 4th branchial anomalies, 2nd branchial cleft fistulae/sinuses are found along the anterior border of sternocleidomastoid. A fistula tracks deep to platysma (embryologically covers external opening of Sinus of His) and courses superiorly between the internal and external carotid arteries and passes over the XIIn and IXn to enter the supratonsillar fossa (Figure 6). A cyst may occur anywhere along its course.
A 2nd branchial cleft cyst typically presents as a mass along the anterior border of sternocleidomastoid (Figures 8, 18, 19). It contains a clear fluid and transilluminates with light.
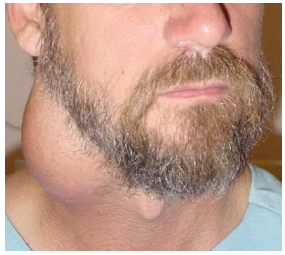

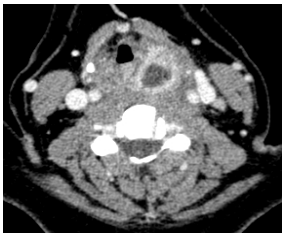
It is clinically indistinguishable from other conditions such as a Level 2 cystic metastasis from carcinoma of the oropharynx, skin or thyroid (Figure 20) and from salivary and hydatid cysts in the parapharyngeal space. Therefore it is important in the adult to examine the upper aerodigestive tract for a primary cancer and to send a fine needle aspirate for cytologic examination.
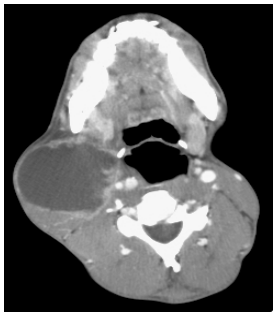
The branchial cyst +/ tract is surgically excised under general anaesthesia. CT or MRI may help to delineate a tract (Figures 15-17). Tonsillectomy may be required if the tract terminates in the supratonsillar fossa. Avoid operating on an inflamed cyst; aspirate the contents, commence antibiotics and adjust the choice of antibiotics in accordance with the microbiology results of the aspirate.
Third and 4th branchial cleft cysts are rare. Because of their common origin from the Sinus of His, 3rd and 4th branchial cleft cysts share certain features. They typically present as recurrent cervical abscesses or are misdiagnosed as acute suppurative thyroiditis (Figure 27). An external sinus or fistula is located along the anterior border of sternocleidomastoid (Figure 27). Because the 2nd - 4th clefts jointly form the Sinus of His with a single external opening, it is impossible to distinguish branchial clefts 2 - 4 from one another based on the location of a skin sinus or fistula.
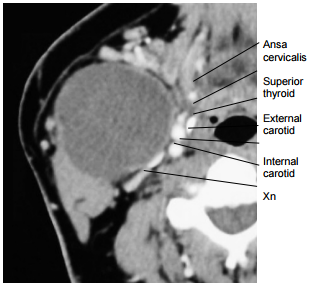
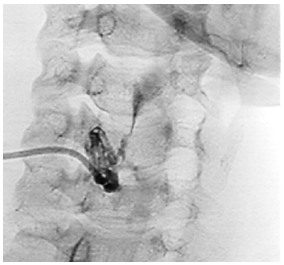
The cleft or pouch of origin is defined by the location of the internal (pharyngeal) opening. Unlike 2nd branchial anomalies, 3rd and 4th anomalies enter the pyriform fossa below the level of the hyoid bone (2nd arch). Gas in the region of the upper pole of the thyroid gland abutting the pyriform fossa on ultrasound or CT is pathognomonic of 3rd or 4th branchial anomalies. Barium oesophagogram has a high sensitivity for demonstrating the internal opening of a fistula in the pyriform fossa. Fluoroscopic or CT sinogram/ fistulogram may delineate the course of a tract (Figure 28).
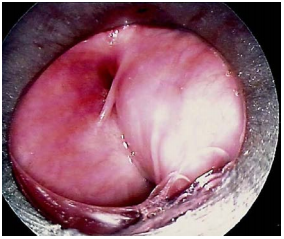
Direct laryngoscopy will reveal the internal opening of a sinus or fistula in the pyriform fossa (Figure 29).
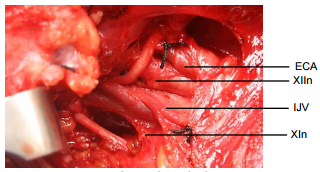
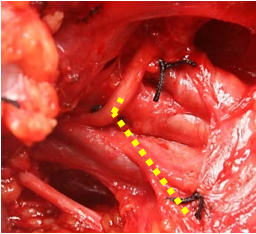
A fistula tracks deep to platysma, passes behind the internal carotid artery, loops over XIIn, courses just superior to the superior laryngeal nerve to pierce the thyrohyoid membrane and enters the upper part of the pyriform fossa. Branchial cysts may occur anywhere along the course of this tract (Figure 30).
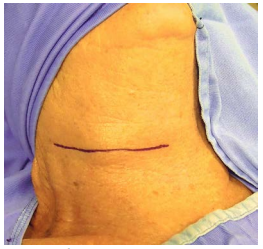
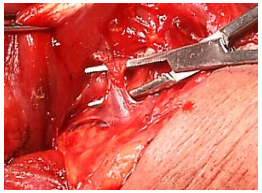
Resection is via a transverse skin crease incision or via thyroidectomy approach. Be prepared to have to identify the recurrent laryngeal nerve and to do partial thyroid lobectomy. Superiorly preserve the superior laryngeal nerve where it traverses the thyrohyoid membrane (Figure 31).
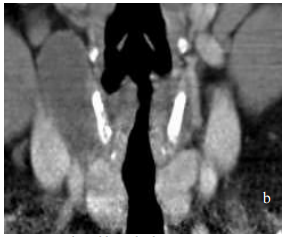
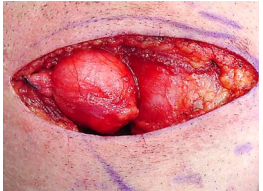
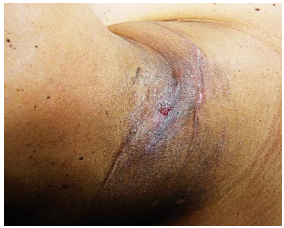
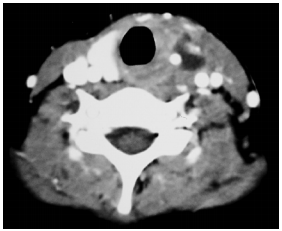
These are extremely rare. They almost always occur on the (L) side and typically are misdiagnosed as “acute suppurative thyroiditis”, or cervical abscesses that have been repeatedly drained (Figures 32, 33).
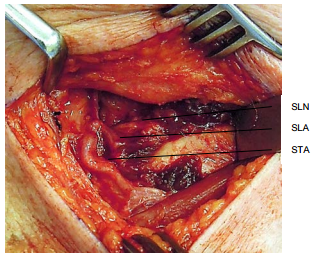
The external opening of a fistula or sinus is found along the anterior border of the sternocleidomastoid and is generally a con sequence of incision and drainage of a branchial cyst that has been mistaken as a “cervical abscess”. The diagnosis is clinched by finding an internal opening near the apex of the pyriform fossa on direct laryngoscopy (Figure 29).
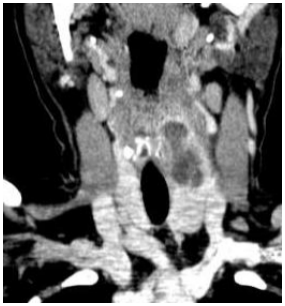
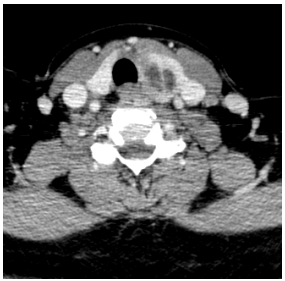
A true fistula would follow the course of the recurrent laryngeal nerve around the aorta (left) or subclavian artery (right), to then ascend superficial to the recurrent laryngeal nerve in the paratracheal region; this has never been reported in practice. It then passes behind the thyroid ala and opens into the apex of the pyriform fossa; 4th branchial cleft cysts may occur anywhere along this course including abutting thyroid gland and within the mediastinum (Figures 6, 29, 32-37).
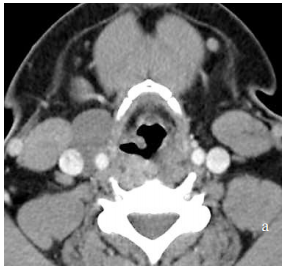
CT scan is an important investigation as it is both diagnostic and serves as a surgical roadmap. CT-fistulography may delineate the fistula tract.
Treatment is to excise the cyst and/or fistula, and is often combined with partial thyroidectomy (Figures 35-37).
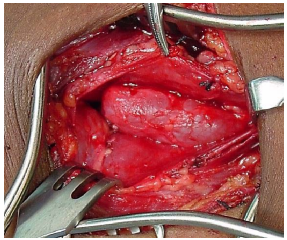
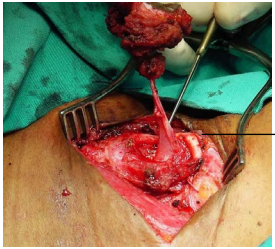
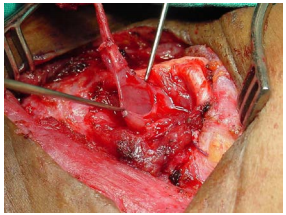
Partial resection of the thyroid lamina may be required to gain exposure to where the tract enters the pyriform fossa (Note: an entire thyroid lamina may be resected without causing functional problems). Although the fistula tract theoretically extends into the mediastinum, this is rarely the case in clinical practice.
Endoscopic cauterisation of the sinus opening and tract in the pyriform fossa has been described (Verret et al). At direct laryngoscopy an intravenous balloon catheter or angiocath is advanced into the sinus tract at the apex of the pyriform fossa; the balloon is inflated to dilate the opening of the sinus and an electrocautery ball coagulator is inserted into the sinus opening and the tract is coagulated.
Chemocauterization with 40% trichloroacetic acid (TCA) is less invasive and has been proposed as 1st line treatment, although patients may be prone to recurrence (Cain et al). The purported advantages of TCA over electrocautery are that a longer segment of tract can be obliterated without risk of thermal injury to adjacent structures. It can be repeated several times, where after surgery is recommended for recurrence.
Johan Fagan MBChB, FCORL, MMed
Professor and Chairman
Division of Otolaryngology
University of Cape Town
Cape Town
South Africa
johannes.fagan@uct.ac.za