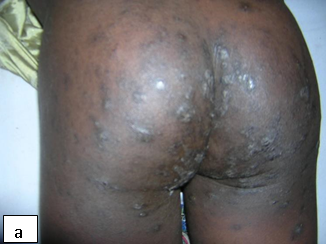
Description:The clinical presentations of scabies include papular, nodular, bullous and crusted scabies.
Aetiology: Scabies is caused by a mite (Sarcoptes scabiei var homini) and has an incubation period of about three weeks.
Clinical presentation: Presents with Itching (severe at nights), characteristic burrow in the interdigital web spaces, papules, blisters, nodules, and eczematous changes. The skin lesions commonly involve web spaces, flexor surface of wrists, axillae, umbilicus, waist, feet, and ankles. In HIV-infected children it can affect the face, scalp and nail folds. Crusted or Norwegian scabies is mainly seen in immunosuppressed individuals such as patients with HIV/AIDS. It is highly contagious and may be the source of epidemics.
Epidemiology: An estimated 300 million cases per year occur worldwide. It is associated with overcrowding and poor sanitary conditions. Epidemics can occur among children in institutional care. Mode of transmission is mainly through direct contact.
Diagnosis: Clinical diagnosis can be made but definitive diagnosis is made by microscopic identification of mites, eggs, or mite faeces (scybala) from skin scrapings.
Prevention: Personal hygiene. Prompt diagnosis and effective treatment. Avoid close contact with infected persons or contaminated fomites.
Treatment: Treat the whole body and all contacts with scabicides. Where available, the commonly used scabicide is benzyl benzoate. If benzyl benzoate is not tolerated, sulphur ointment is used. For children <6months of age: 5% sulphur ointment twice daily for 3 days; 6 months – 2 years of age: ¼ strength benzyl benzoate as a single application; 2 – 12years of age: ½ strength benzyl benzoate as a single application and >12 years of age: full strength benzyl benzoate as a single application. Permethrin and ivermectin are alternative therapy: 200mcg/kg in two divided doses given 2 weeks apart. In crusted scabies oral ivermectin is best combined with a topical scabicide. It is useful to remember that the scabies mite can only live about 72 hours without human contact, but once on a person, the mites can live up to two months.
Tetmosol soap is added to wash the body, clothes and linen.
Complications: Secondary bacterial infection can occur.

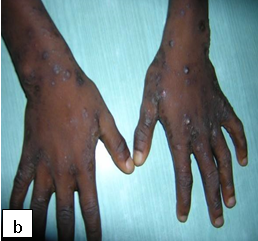
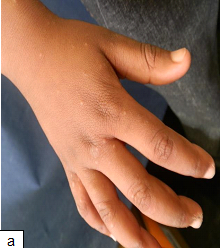
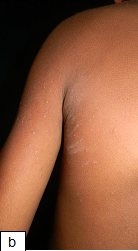
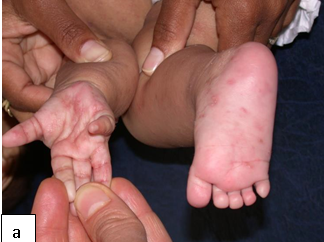
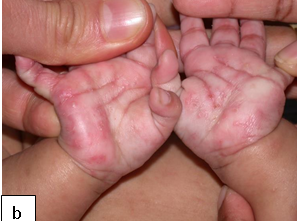
Description: Pediculosis is infestation of the hairy parts of the body by lice.
Aetiology: Head lice are caused by Pediculus humanus capitis while pediculosis pubis causes infestation of the public area
Clinical presentation: Itching on the affected area 3-4 weeks after infestation
Epidemiology: A common parasitic infection in children and most prevalence in children between 3 and 11 years old. It is rare in African children due to the texture of their hair. There is no seasonal variation or relationship with the level of hygiene.
Diagnosis: Pediculosis is diagnosed by identifying live lice on the affected area.
Prevention: Health education. Avoid physical contact with infested persons and their materials such as beddings, clothing and comb.
Treatment: There is no modality that assures destruction of the eggs and hatched lice after a single treatment. Options include physical methods (wet combing), topical pediculicides (pyrethrins, pyrethroids pyrethrins, and lindane). Treatment should be repeated after an interval of 7-10 days. All other contacts should also be treated.
Complications: Secondary bacterial infections.
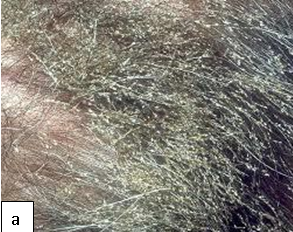

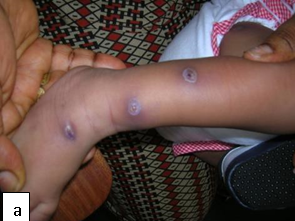
Description: Myiasis manifests as boil-like lesions, usually on exposed areas of the body such as the trunk, thigh and buttocks.
Aetiology: The lesions are caused by infestation of the skin by developing larvae (maggots) of the tumbu fly (Cordylobia anthropophaga). The female fly lays its eggs on dry, sandy soil or on damp clothing hung out to dry. The eggs hatch in 1 to 3 days and penetrate the skin.
Epidemiology: The tumbu fly is prevalent in sub-Saharan Africa, thriving in the warm and humid environment. Myiasis occurs more commonly in children and during the raining season. Clinical presentation: Lesions can be painful, pruritic, and tender, and patients often have the sense of something moving under the skin. There may also be fever or swollen glands. In ophthalmomyiasis, there may be severe eye irritation, redness, foreign body sensation, pain, lacrimation, and swelling of the eyelids.
Diagnosis: Each lesion has a central punctum from which serosanguinous fluid may be discharged and the movement of the larva may be noticed by the patient. The tip of the larva may protrude from the punctum. Diagnosis is typically made by identification of the larvae. Ultrasonography may be useful in establishing the diagnosis and in determining the size of the larvae. Biopsies are not usually necessary.
Treatment: A non-invasive mode of management is to occlude and suffocate the larva by application of petroleum jelly or liquid paraffin over the central punctum. This makes the larvae to emerge spontaneously head-first over the course of several hours, at which time, tweezers (or forceps) aid in the removal.
Prevention: Clothing should be hot-ironed and dried appropriately to remove any residual eggs in areas endemic to tumbu flies.

| Condition | Treatment1 | Treatment2 | Treatment3 |
|---|---|---|---|
| Scabies | Benzyl benzoate | Ivermectin | Permethrin |
| Pediculosis | Physical methods (wet combing) | Choice of pyrethrins, pyrethroids, lindane | Oral antihelminthics and antibiotics |
| Myaisis | Petroleum jelly or liquid paraffin over the central punctum |