Metacarpal and phalangeal fractures
by Neil Kruger, Pieter Jordaan & Duncan McGuire
Learning Objectives
- The majority of metacarpal and phalangeal fractures can be managed non-surgically.
- It is a myth that all phalangeal fractures can be managed with buddy-strapping only.
- Open hand fractures should be managed the same as all other open fractures.
- Never splint the metacarpophalangeal joint (MCP) in extension.
Definition
A fracture is defined as a cortical discontinuity of bone, resulting in compromising the normal mechanical properties.
Background
Almost all fractures of the metacarpals and phalanges result from direct or indirect blunt or sharp force trauma. In rare circumstances, the underlying bone may be pathological (due to a disease process such as infection or tumour) and fracture when lesser forces are applied.
Common fractures of the metacarpals include:
- The base (which may occur with dorsal dislocation of the metacarpal relative to its proximal articulating carpal bone. Be sure to always check the lateral X-ray for this).
- The shaft.
- The metacarpal neck (classically the ‘boxer’s fracture’ of the 5th metacarpal due to a punching mechanism).
Phalangeal fractures can occur in the proximal, middle or distal phalanx. Fractures in these locations are described according to their soft tissue covering (open or closed), morphology (transverse, oblique, or comminuted), and the site of the fracture (base, shaft or head).
When deciding on management, it is essential to define the amount of shortening, angulation (in the sagittal and coronal plane) and rotation and apposition (percentage of bone ends in contact). These form part of the decision to offer surgery or conservative management.
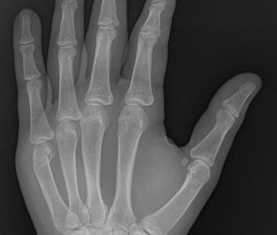
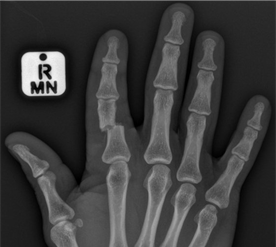
Clinical findings
History
The history is usually straightforward, with a specific incident of acute trauma. Remember to do a thorough secondary survey down to fingers and toes in polytrauma patients, as fractures of the hands and feet are commonly missed when concentrating on life-threatening injuries.
Examination
Often the deformity is obvious, with severe pain and swelling present. If in doubt, gentle palpation will cause pain, with crepitus and movement at the fracture site. Look very carefully for open wounds and treat any open wound in the setting of a fracture as an open fracture; never assume that the wound does not communicate with the fracture. Do a careful neurovascular examination and check for tendon injuries.
No degree of rotation is acceptable. The best way to assess rotation is to flex the joint distal to the fracture to 90° gently and compare the alignment to the neighbouring fingers. Alternatively, all fingers should point towards the scaphoid tubercle with full flexion of the MCP and proximal interphalangeal (PIPJ) joints.
Special investigations
Imaging
X-ray is mandatory in clinically suspected fractures to confirm the diagnosis and define the fracture morphology to help decide on treatment. Occasionally CT scans are required in the case of complex fractures.
Management
Metacarpal fractures
Management depends on whether the fracture is open or closed, whether intra- or extra-articular and on the displacement. If open, it requires a thorough debridement in theatre, and then mostly some form of stabilisation is needed, depending on the fracture morphology and location. In open injuries, remember to look for lacerations of tendons, vessels and nerves specific to the site of injury.
If closed and intra-articular, an open reduction is required to restore the congruity of the joint surface.
If closed and extra-articular, management is decided according to the displacement (length, alignment, rotation and apposition).
For all closed extra-articular metacarpal fractures, the values for conservative treatment of a fracture are:
- Length:<2–5mm loss of height.
- Apposition: >50% apposition.
- Rotation: No rotation.
- Alignment: Depends on the finger involved and the position of the fracture.
An easy way to remember is for shaft fractures, from index to little finger the acceptable angulations are up to 10°, 20°, 30° and 40° respectively. From index to little finger, they are the same for neck fractures, except the little finger can tolerate up to 60° of angulation.
Conservative management involves a splint and buddy taping. Generally, the metacarpophalangeal joints can be left free and motion encouraged to prevent stiffness. The fracture characteristics dictate operative management, and if needed, an open reduction and internal fixation are performed with K-wires, plates or screws.
Phalangeal fractures
Phalangeal fracture management is similarly determined by whether they are open or closed, intra- or extra-articular and on the degree of displacement.
If open, it is treated with the same principles as for a metacarpal fracture and then mostly with subsequent fixation, either using K-wires, screws or a plate if necessary.
If closed and intra-articular, unless undisplaced, it requires open reduction and internal fixation to restore articular congruency.
If closed and extra-articular, the management is decided on by the displacement.
Acceptable parameters are:
Length: <2mm shortening
Apposition: >50% apposition
Rotation: None
Alignment: <20° in any plane
If the position is not acceptable, the fracture can be reduced under ring block, splinted (see below) and a check X-ray performed.
When treating proximal phalanx fractures conservatively, they are reduced and immobilised in a dorsal backslab with the MCPJs pushed to maximal flexion and the IPJs held in full extension until the cast is hard. This is important because the natural deforming forces will pull the distal fragment into extension, which will lead to a malunion if the MCPJ is not fully flexed. Active flexion of the IPJs should be performed in the cast to prevent stiffness. If a hand therapist is available, a splint can be used. Middle phalanx fractures can be managed similarly. Distal phalanx fractures are usually best treated in a splint immobilising the distal interphalangeal (DIP) joint.
In all conservatively managed fractures, remember to do check X-rays after one week to check for loss of reduction.
Pitfalls
- Missing open fractures.
- Missing associated tendon, nerve or vascular injuries.
- Not assessing rotation correctly.
- Splinting the MCPJs in extension, leading to extension contractures.
- Assuming a proximal phalanx fracture is stable and therefore only buddy strapping it, leading to malunion.
References
Hammert WC, Calfee RP, Bozentka DJ, Boyer MI, 2010. ASSH Manual of Hand Surgery; Lippincott, Williams and Wilkins (Wolters Kluwer); Philadelphia, USA.
Miller MD, 2008. Review of Orthopaedics, 5th edition; Elsevier; Philadelphia, USA.
Wolfe SW, Hotchkiss RN, Pederson WC, Kozin SH, Cohen MS, 2017. Green’s Operative Hand Surgery, 7th Edition; Elsevier; Philadelphia, USA.
Assessment
A young male patient fell and sustained a closed fracture of his index finger proximal phalanx. You give him a ring block for analgesia and ask him to make a fist. His index finger overlaps his middle finger. The ideal management is:
- Buddy strap index to the middle finger and see in three weeks.
- Buddy strap and apply a dorsal splint with the wrist slightly extended, the MCPJ maximally flexed and the IPJs in extension.
- Reduce the fracture, buddy strap and apply the same splint as in ‘b’ and get a check X-ray to confirm the position.
- Refer to physiotherapy for mobilisation.
- Refer the patient immediately.
The correct answer is (D), reduce the fracture, buddy strap and apply the same splint as in ‘(B) and get a check X-ray to confirm the position.