Thumb base/carpo-metacarpal joint osteoarthritis
by Pieter Jordaan, Neil Kruger & Duncan McGuire
Learning objectives
- Common and debilitating cause of thumb pain in the elderly.
- Diagnosis is clinical but confirmed with X-ray.
- Early disease can be treated conservatively.
- Advanced disease or failed conservative measures require referral.
- Treatment is symptomatic and for pain relief.
Definition and anatomy
Osteoarthritis between the trapezium and thumb metacarpal.
Causes and associations
This is generally a degenerative condition but can be seen after trauma in younger patients. The disease is more common in postmenopausal women. It is the second most common site of osteoarthritis in the hand behind the finger distal interphalangeal joint.
Differential diagnosis
- De Quervains’s tenosynovitis.
- Scapho-trapezio-trapezium (STT) joint arthritis.
- Rheumatoid arthritis.
Diagnosis
History
Patients present with radial-sided wrist pain or pain at the base of the thumb aggravated by loading the joint, such as trying to open a jar or tap and writing.
Examination
The hand can appear normal, but usually, the base of the thumb appears squared off (the metacarpal base is subluxated), with adduction of the thumb. In advanced cases, the thumb MCP-joint will be hyperextended.
There is tenderness over the joint line with decreased range of motion
Special test
Grind test – reduction of the thumb, with gentle downward pressure on the base of the thumb metacarpal, combined with axial loading reproduces the pain.
Special investigations Imaging
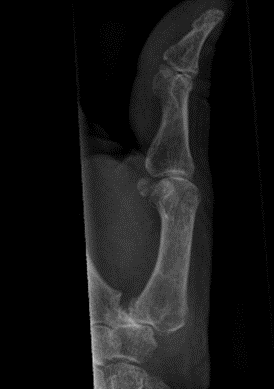
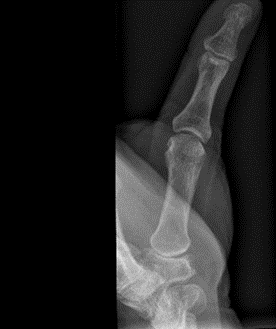
An X-ray can be used to confirm the diagnosis. Views of the base of the thumb, including a PA, lateral, and Robert’s view (hyper-pronated) should be done. This will show subluxation of the carpometacarpal joints (CMCJs), with joint space narrowing, sclerosis, osteophytes and cysts.
Management
Non-surgical
First-line therapy is rest and NSAIDs and referral to a hand therapist for lifestyle modification and assistive devices. They can also provide the patient with a splint, which is very effective. If this fails, the patient can be offered an intra-articular steroid injection.
Surgical
Failed conservative measures or advanced severe disease will require surgery. There are many options, but the most reliable results are achieved with a trapezium excision with or without ligament reconstruction and tendon interposition, specifically in older, less active patients with advanced disease. Arthroplasty is an option but is not proven to be better than trapezium excision in the long term.
Post-traumatic arthritis in manual labourers will do better with a fusion of the CMCJ joint, and in young patients with early disease, a metacarpal osteotomy can be performed.
References
Hammert WC, Calfee RP, Bozentka DJ, Boyer MI; 2010; ASSH Manual of Hand Surgery; Lippincott, Williams and Wilkins (Wolters Kluwer); Philadelphia, USA.
Miller MD; 2008; Review of Orthopaedics, 5th edition; Elsevier; Philadelphia, USA.
Wolfe SW, Hotchkiss RN, Pederson WC, Kozin SH, Cohen MS; 2017; Green’s Operative Hand Surgery, 7th Edition; Elsevier; Philadelphia, USA.
Assessment
A 67-year-old female patient presents with radial-sided wrist and thumb pain. She is unable to open her honey jar at home. Her thumb appears adducted, and squaring is noted at the base of the thumb metacarpal.
Which of the following will be the best to confirm your suspected diagnosis?
- Full blood count and ESR.
- Finkelstein test.
- Ultrasound.
- PA and lateral X-ray of the thumb.
- PA, lateral and Robert’s view of the thumb.
The correct answer is (E), PA, lateral and Robert’s view of the thumb.